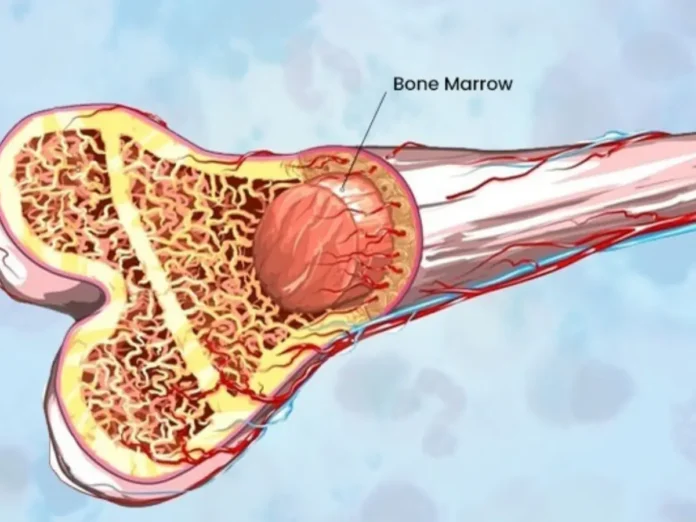
Bone marrow is the “blood factory” of the body, located inside the bones. It is responsible for producing red blood cells (oxygen carriers), white blood cells (infection fighters), and platelets (clotting agents). When this factory fails, the body becomes vulnerable to a range of life-threatening issues.
The Three Red Flags
According to Dr. Pawan Kumar Singh, Vice Chairman of Haemato-Oncology & BMT at ShardaCare Healthcity, patients should look for a combination of these three signals:
- Anemia (Low Red Blood Cells): Results in chronic fatigue, pale skin, dizziness, and shortness of breath.
- Leukopenia (Low White Blood Cells): Leads to recurrent infections, frequent fevers, and slow recovery from minor illnesses.
- Thrombocytopenia (Low Platelets): Causes easy bruising, frequent nosebleeds, or bleeding gums.
Who is at Risk?
While bone marrow failure can be idiopathic (of unknown cause), certain factors increase the risk:
- Environmental Exposure: Prolonged contact with toxic chemicals, pesticides, or radiation.
- Medical History: Previous chemotherapy, viral infections, or autoimmune diseases.
- Genetics: A family history of blood disorders.
- Demographics: While it can affect anyone, it is frequently seen in children, young adults, and the elderly.
Why Early Detection Matters
The danger of bone marrow failure lies in its subtlety; symptoms often appear gradually and worsen over time. Dr. Singh emphasizes that early specialist evaluation—specifically by a hematologist—is vital.
Early-stage treatment can range from medication and immune-based therapies to supportive care. In advanced or late-detected cases, a bone marrow transplant may be the only curative option.